The Clinic: Jon Rogers & Answers To The 4 Most Common Questions About Spinal Stenosis
The Clinic: Jon Rogers & Answers To The 4 Most Common Questions About Spinal Stenosis https://bestpracticehealth.tv/wp-content/uploads/2022/01/My-Post-copy-2-1024x576.jpg 1024 576 Best Practice Health TV Best Practice Health TV https://bestpracticehealth.tv/wp-content/uploads/2022/01/My-Post-copy-2-1024x576.jpgJon Rogers and his wife moved to Phoenix to start a new life. Trained as an aerospace engineer, Jon worked on some of the largest military projects in America. For example, Jon was on the team that developed the Top Gun missile for the US Air Force.
When it came time to retire, he moved to Tucson with his wife to start his second act as a cowboy. He absolutely loved the Marlboro man. Jon rode his horse and put up a Marlboro poster in the recreation of Tombstone he had built in his backyard. However, over time, the couple started having problems.

They decided to leave the horses behind and move to Phoenix. Unfortunately, Jon’s health issues followed them.
If Jon didn’t have all this trouble with his back and brain, his wife was ready to enjoy retirement and go on a long-awaited cruise. The couple is still in hopes of fixing Jon’s medical problems so they can finally be on the big boat this coming Spring.
What does spinal stenosis feel like?
The hallmark of spinal stenosis is pain or heaviness in the legs with walking; there may be associated electrical pain as well as back ache. The pain with walking, electrical sensation, and backache are all relieved particularly by bending over, as well as resting in general.
Jon’s description of his symptoms is the classic picture of spinal stenosis. “It starts in my back and then goes all the way down my legs.” Everyone is different; however, anyone with spinal stenosis will have some combination of:
1.) Pain down the legs while walking
Spinal stenosis constricts the space around the nerve roots in the spinal canal which causes pain down the legs while walking. The electrical pain, or fullness you feel in the legs while walking, is relieved by bending forward. That is because by bending forward, the spinal canal opens up and makes more room. People with spinal stenosis can often become aware of it first in the grocery store; if they lean on a cart, they can walk further.
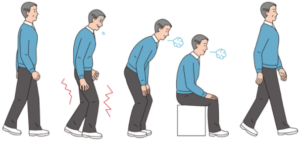
2.) Nerve root problems with weakness, numbness, and loss of reflexes
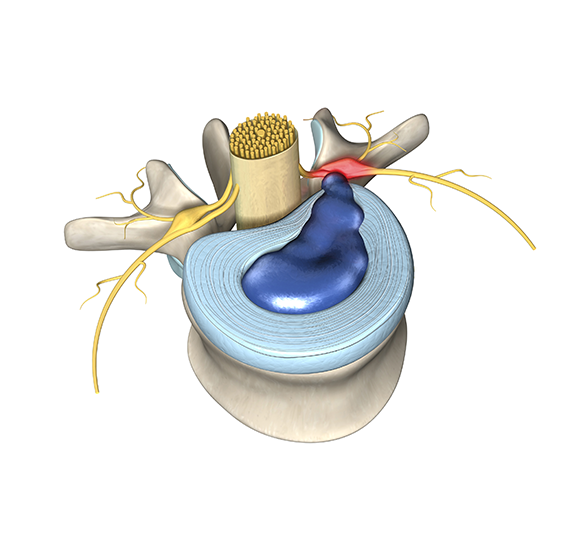
In addition to pain with walking, spinal stenosis causes pain to shoot down the leg. Narrowing of the side of the spinal canal, or of the passages through which the nerve roots pass, causes nerve root compression. You feel a shooting pain in the area controlled by the compressed nerve root. Your doctor may find numbness and weakness on examination as well.
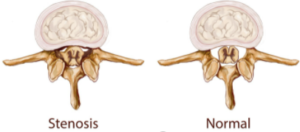
3.) Low back pain
Spinal stenosis also causes back pain that feels just like an arthritic joint, complete with the muscle spasm and ache.
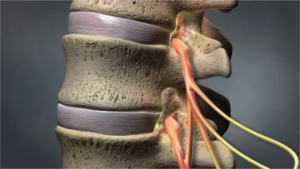
Is spinal stenosis a serious condition?
Spinal stenosis is extremely serious. Lumbar spinal stenosis, such as Jon presented with, will persistently worsen. If left untreated, spinal stenosis will cause paralysis of the legs, uncontrollable pain while standing/walking, numbness in the legs, inability to control ones bladder, and sexual dysfunction.
Before the modern laminectomy surgery came around, the result of spinal stenosis was paralysis , incontinence, and sexual dysfunction that oftentimes led to lethal urinary tract infections. Today, we do not let that happen.
The truth is, you cannot know if you have spinal stenosis based solely on how it feels. Clogged arteries can be another reason for pain shooting down your leg while walking. Bad veins can make your legs feel heavy. Herniated discs or bone spurs can also cause pain down your leg. You may suspect you have spinal stenosis due to numbness, heaviness, or tingling in your feet when you walk that is relieved by bending over; however, you cannot simply feel spinal stenosis. Spinal stenosis is confirmed by getting an MRI.
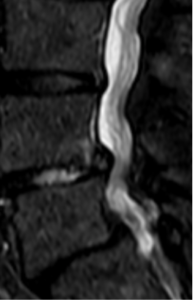
This is a sagittal cut through Jon’s low back taken with magnetic resonance imaging. In this cut, the square blocks are the vertebral bones. The spinal fluid in the spinal canal is white. In the upper third of the picture, look in the white spinal canal as you can appreciate “strings” running from top to bottom of the image. Those strings are the spinal nerve roots inside the spinal canal. About mid-way in the image, you see the white area narrows. This is spinal stenosis.
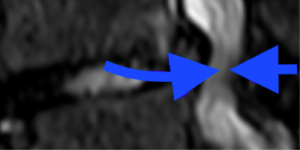
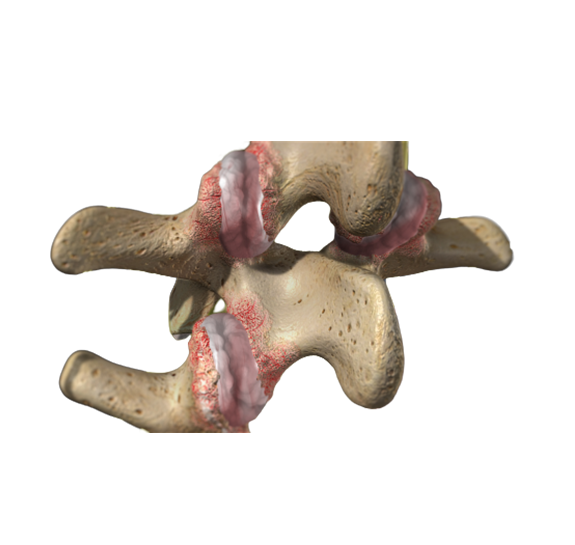
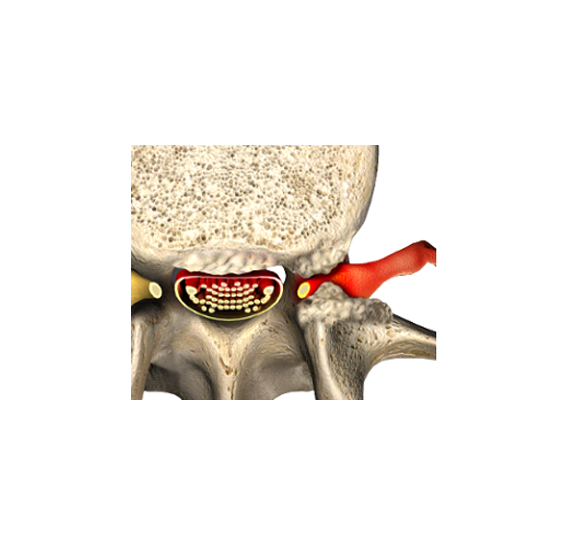
Spinal stenosis is caused by several factors. Discs form the floor of the spinal canal (left arrow), so a bulging disc means your floor is rising. The right arrow shows a ligament under the lamia bone. With age and wear ligament thickens. This means the roof is coming down. The spinal bones are also shifted slightly, trapping the spinal canal in between.
The term ‘stenosis’ refers to narrowing of the spinal canal which holds the spinal cord (cervical and thoracic). Your nerve roots get their oxygen from the fluid around them. Severe narrowing of the canal restricts the fluid so the nerve roots cannot get the oxygen they need when you walk. Think of the spinal canal as a room: the roof is the ligament, the walls are the facet joints, and the floor is the disc space. The ligament thickens with age because of wear and tear. And discs are famous for “bulging” (Herniated Disc). As a result of all these changes, with age and the roof coming down, the walls are moving and the floor is rising. Joints normally get bigger with age. (If you do not believe it, and you are over 40, look down at your knuckles.) It is not a surprise, then, that the spinal canal is getting smaller.
Some people do not need to wait; they are born with a very narrow spinal canal. This condition is called congenital spinal stenosis. You know you have it if one of your parents and your siblings have already had Laminectomy surgery. You can also develop narrowing of the spinal canal due to a shift in the vertebrae. The spine is a rigid ring. If one band moves forward on the other one, it creates a kink in between. This type of movement is called spondylolisthesis.
See the problem? Once it gets started, the processes of spinal narrowing can only get worse. Spinal stenosis is always progressive; it only gets worse. That means there is no stretching, exercise, injection, medicine, magic crème, or supplement that can help. Even sleeping in a pyramid with magnetic walls will not save you. We know this through countless studies.
Can Stenosis of the spine be cured?
Spinal stenosis can be cured by laminectomy surgery. In Jon’s case, he has severe narrowing evident on MRI that is causing pain in the legs with walking. Jon was therefore referred for laminectomy surgery; however, he must deal with the normal pressure hydrocephalus in his brain first. If you are medically fit to undergo general anesthesia, have pain down the legs while walking, and MRI shows moderate to severe narrowing of the spinal canal, then you are a suitable candidate for laminectomy surgery.
Beware! The internet is full of claims for exercises, stretches, and things you can take to avoid surgery with spinal stenosis. The only thing that can make all small hole bigger is surgery. The rest of these claims are nonsense.
The roof of the spinal canal is a bone called the lamina. In medicine removing something is an –ectomy. For example, if they take out your tonsils you would call that tonsillectomy. Similarly, raising the roof of the spinal canal is an operation called laminectomy, which means “removing the lamina”. At the Phoenix Spine & Joint Surgery Center our surgeons perform laminectomy on patients with spinal stenosis using a “minimally invasive” approach. They make a 1/2-inch incision in the skin, and under x-ray guidance, insert probes which gently dilate the muscles away from the lamina bone. Looking down the microscope, through a retractor, they then drill off the lamina bone, and then remove the ligament. When necessary, we can remove herniated disc material at the same time. The operation usually takes between 30 and 60 minutes. It is done on an outpatient basis.
Most people are recovered from laminectomy surgery in 3 days, and fully recovered in a week. There are restrictions after surgery. You should try not to bend, lift, or twist with more than 5 pounds for the first 3 weeks. Most patients can lift 20 pounds after 3 weeks, and 40 pounds after 6 weeks (about 1 and a half months). After 12 weeks (about 3 months) there are no restrictions. We have an extensive home exercise program we advocate for all patients. If you are unable to start out in our program, physical therapy may be needed as a bridge. Most of our patients are back to light work after a week, moderate duty after 3 weeks, and heavy work after 12 weeks (about 3 months).
The benefit of laminectomy surgery was established in a randomized, controlled trial reported in The New England Journal of Medicine in 2008. Read about the study here:
This was a randomized, controlled trial involving 13 medical centers and hundreds of patients. The study was paid for by the National Institutes of Health (US Federal Government), so there was no financial bias in the outcome. The authors found that patients who had surgery did substantially better than those who did not have surgery. In addition, the study was hard to conduct because so many patients randomized to NOT have surgery ended up insisting on having surgery.

Laminectomy surgery is…
- Found to be worth the risk by studies tracking outcomes
- Liked by over 94% of patients when done using the right minimally invasive approach
- Recommended by doctors in practice for their patients
- Paid for by Private health insurance companies and Medicare as standard of care
What is the best treatment for spinal stenosis?
The best treament for spinal stenosis is laminectomy surgery. Laminectomy surgery is the only treatment available that decompresses the spine. However, not everyone can have surgery. The most common alternatively to surgery for the management of spinal stenosis are:
- Medications – mostly NSAIDS and opioids
- Physical therapy
- Epidural steroid injections
Until 2014 pain management doctors gave epidural injections for the treatment of early spinal stenosis. Then, a group of doctors tested it: Injections for Spinal Stenosis
Trials can be done in several ways. The worst way to do a trial is called a case series. That is where a surgeon says, “I did this and this and that, and here’s what happened.” The problem with this kind of process is bias and lack of transparency. We do not know how patients were selected, how many were rejected, and how much of the effect observed was due to placebo. The style of trial with the least bias and that provides the strongest results is a randomized controlled trial. That is where people with spinal stenosis would be assigned by flipping a coin to injection or no injection.

The randomized trial showed no benefit to epidural injection for spinal stenosis. As a result, the doctor concluded that:

To watch Jon Rogers whole story, and learn more about spinal stenosis, visit:

- Post Tags:
- Pg - Laminectomy
- Pg - low back fusion
- Posted In:
- Herniated Disc With Sciatica
- Low Back Pain