A New Alternative to Fusion Surgery: Direct Visual Rhizotomy
A New Alternative to Fusion Surgery: Direct Visual Rhizotomy https://phoenixspineandjoint.com/wp-content/themes/psjoints/images/empty/thumbnail.jpg 150 150 Phoenix Spine & Joint Phoenix Spine & Joint https://phoenixspineandjoint.com/wp-content/themes/psjoints/images/empty/thumbnail.jpg If you’re one of the millions of Americans who suffer from pain in your low back, you should know that there may be a solution. In most cases, mechanical back pain is caused by problems with a facet joint. It’s often called arthritis of the spine. The traditional treatment for this problem is radiofrequency ablation (burning of the nerves) or a fusion. Unfortunately, neither of these common procedures is a really good solution for facet joint pain. Here’s why.
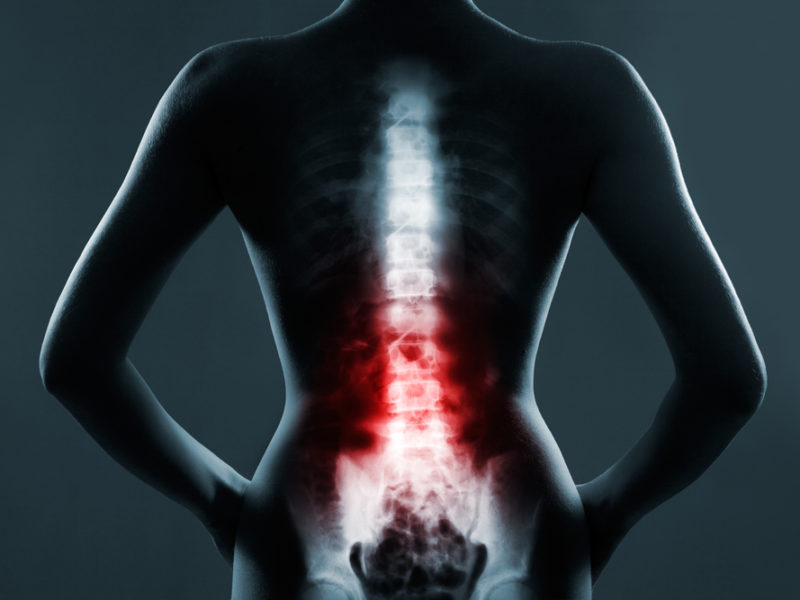
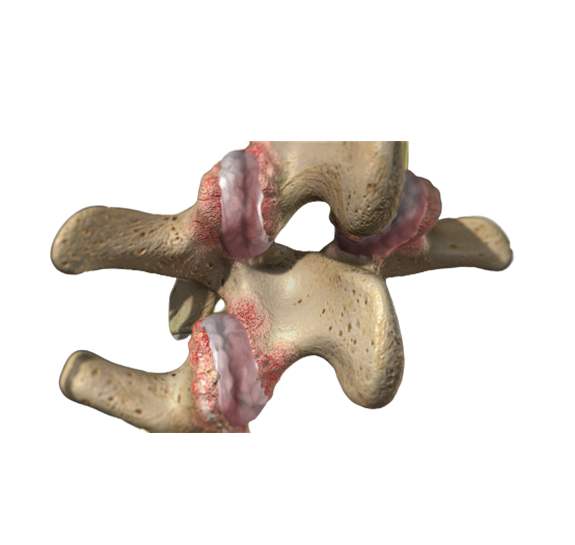
If you’re one of the millions of Americans who suffer from pain in your low back, you should know that there may be a solution. In most cases, mechanical back pain is caused by problems with a facet joint. It’s often called arthritis of the spine. The traditional treatment for this problem is radiofrequency ablation (burning of the nerves) or a fusion. Unfortunately, neither of these common procedures is a really good solution for facet joint pain. Here’s why.
Fusion
Fusion surgery is invasive, permanent, and often needs to be repeated. The bone healing involved in a fusion surgery takes six-12 months to heal completely. Most fusion surgeons these days place hardware in your body to fixate the spine. Long hospital stays, blood transfusion, infection, persistent pain, and damage to nerve roots by hardware, broken hardware, and failure to fuse are all painful and very possible complications. Fusion surgery also often leads to the need for more fusion surgeries. In fact, based on prior data we know that 17 percent of the tens of thousands of people who will have a fusion this year will have already had another fusion surgery within the past four years. Fusion surgery is also not reversible; once it’s done, it can never be undone. While fusions may be necessary for the rare case of spinal instability, they’re at best overkill, and at worst dangerous, for many patients.
Radio Frequency Ablation
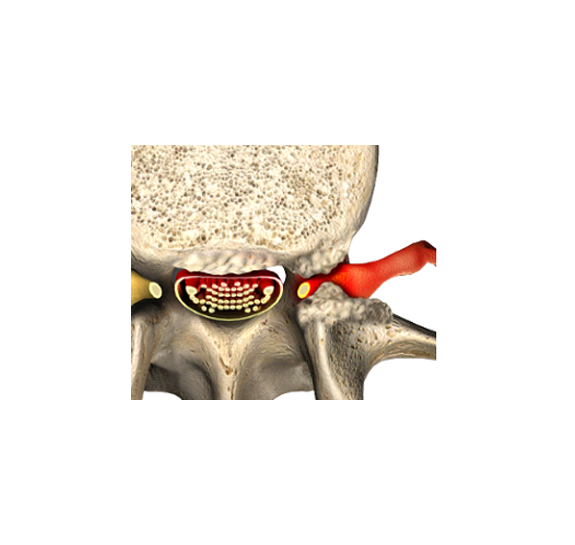
Conversely, radiofrequency ablation (RFA) is rarely enough. The goal of RFA is to relieve back pain using a needle to “burn” the pain fibers that transmits the back pain signal as it comes out of the facet joint. The problem with RFA is that the doctor does not have a direct visual of the nerves he is trying to burn. As a result of working in the dark, only two out of three people can expect to get relief from RFA; and four out of five of them will have the pain come back within six months to a year.
After caring for over 20,000 patients in the last 15 years, I’ve concluded that neither RFA nor fusion is the right solution for most patients with back pain. Fortunately, there is a better way. And it was discovered right here in Phoenix. Dr. Anthony Yeung, a pioneer in endoscopic spine surgery, began experimenting with cutting the pain fibers from the joints in the back almost 10 years ago. Our Direct Visualized Rhizotomy (DVR) procedure has evolved from this approach as the solution to this dilemma.
Direct Visual Rhizotomy (DVR)
DVR is similar to RFA in that it silences your back pain by cutting the pain fibers that transmit the pain signal. Unlike RFA, DVR is done through an endoscope, which is a fiber optic device the size of a straw so he can see through the tip, making it more accurate. The surgeon has a “direct visual” of the nerve during the procedure. A typical DVR procedure takes 10 to 20 minutes, and recovery times are expected to be a few days. Recently, one of our patients at Phoenix Spine woke up from DVR and started dancing with his wife in the recovery room because for the first time in years, he was pain-free!
Won’t cutting the pain fibers cause more damage?
Cutting the pain fibers is not expected to cause numbness, weakness, or any other neurological complication. When DVR began, many patients were concerned that being unable to feel the pain they would further damage their spine. After five years’ experience, we can say there does not appear to be any downside to not feeling pain. There no hardware, blood transfusion, or even hospital stay. DVR is done on an outpatient basis. With DVR, the only thing you have to lose is the pain.
We have completed over 750 DVR surgeries over the last five years. We’ve seen patients who in the past would have risked complications with fusion, or not getting better with RFA, who can now be treated more effectively, safely, and less invasively with DVR. We have also treated dozens of patients who saw limited relief from RFA, but now enjoy complete relief from their debilitating back pain. If you are suffering from facet joint pain, you should know there is a better treatment option.

- Posted In:
- DVR