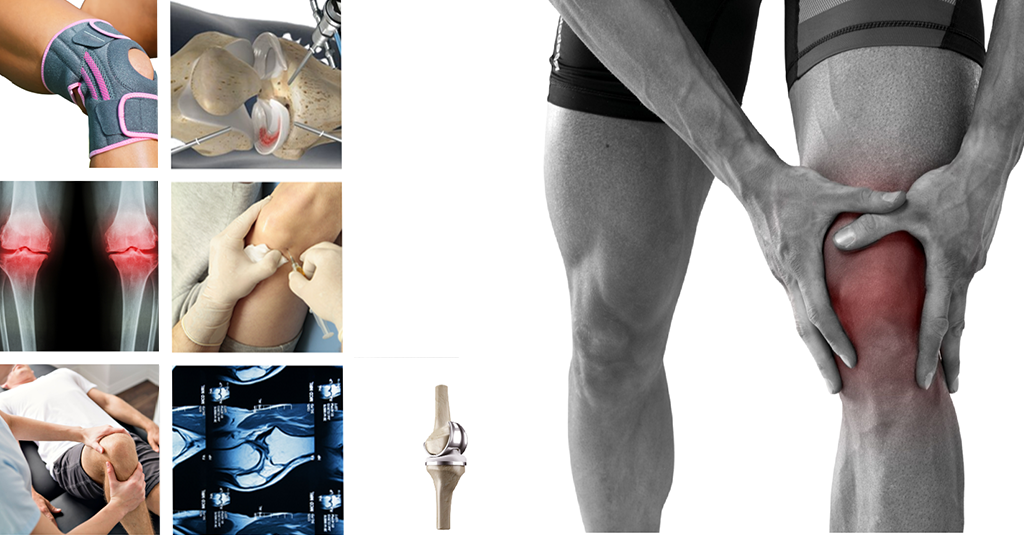
8 Ways To Be Rid Of Knee Pain In the New Year
There may be fifty ways to leave your lover, but fortunately there are only eight things to consider if you have knee pain. With these 8 interventions knee pain can almost always improved and often cured, but you must know where to start. In this article I will walk you through the main options. Most [...]
read more



 Subscribe!
Subscribe!